After four decades, the theory-practice gap in nursing still plagues us.
Four decades!
And after those four decades, today only 23% of new nurses are considered competent and ready to practice. It’s safe to say we haven’t made much progress.
To address the theory-practice gap in nursing head-on, this article discusses the dire consequences and possible solutions to turn things around. After all, we’ve got to start somewhere, right?
A Big Question With Dire Consequences
When you start to think about all the statistics, consequences, and ambiguous terms like “theory-practice gap,” your mind reels. It’s complex. Let’s not get pulled into the weeds just yet. To come up with some quality solutions, it helps to figure out just what the big question is.
The question at the core of the theory-practice gap is pretty simple:
How can we better prepare new nurses for day one of clinical practice?
While simply stated, finding a solution is anything but simple. We haven’t come up with effective solutions to this big question, and now we’re experiencing dire consequences:
- Healthcare patients are endangered.
- Healthcare institutions must use time and resources to bring new graduates up to speed.
- The high turnover rate within the nursing profession continues.
Job loss, endangered lives, stress, money—that’s all at the heart of the theory-practice gap. For more details and graphic statistics like the one below, download a free guide that dives deep into the theory-practice gap in nursing.
What’s Been Tried Before?
Clearly, a lot is on the line with the theory-practice gap, and over the decades, the nursing community has developed lots of strategies and solutions. So what’s been tried before, and what are we currently trying?
An excellent literature review outlines the most promising strategies to address the theory-practice gap in nursing. Some approaches are solely created and implemented by educators. As you’ll see below, nursing programs conjured up quite a few strategies.
Nursing Program Strategies
- Increased use of simulated learning in nursing education
- Disruptive innovations in teaching methods
- Promoting learner-centered, active approaches to learning
- Curriculum revisions
- Competency-based education
Institutions hiring these newly graduated nurses are also trying solutions, and usually, that results in extended orientations or similar programs.
Healthcare Provider Strategies
- Extended orientation for new graduates / Transition to Practice (TTP) Programs
And finally, there are strategies when educators and healthcare providers work together on a solution.
Collaborative Strategies
- Dedicated education units
- Academic service partnerships
All of the listed solutions are promising, but this article will focus first on solutions proposed by nursing programs.
NCSBN Tactics to Prepare New Nurses
For nursing programs, best let the National Council of State Boards of Nursing guide you. The NCSBN identified four trends to answer the big question of how to prepare practice-ready nurses. Here are the four trends:
- Opportunities for experiential learning
- Use of educational technology
- Emphasis on learning outcomes over process
- Evidence-based strategies and curriculum
You may notice that these four points already align with the strategies in the literature review, which means we’re on the right track. As far as the most promising solutions that hit these four trends? No surprise, simulation tops the list.
Using Simulation to Bridge the Theory-Practice Gap in Nursing
It’s like the NCSBN made this list with simulation in mind:
- Experiential learning—check.
- Educational technology—check.
- Emphasis on learning outcomes—check.
- Evidence-based strategy—check.
And these tactics work—studies show time and time again that simulation can better prepare students for the clinical realities they’ll face on the job. That’s why the NCSBN officially announced in 2014 that up to 50% of clinical experiences in core prelicensure nursing courses (the “showing how” and “doing”) can be completed using virtual simulation. 
The key is doing simulation well. Since it’s fairly new, it’s a bit like the Wild West out there. To make sure you’re in line with best practices and state standards, watch a free workshop with INACSL about simulation standards or read “3 INACSL Approved Strategies To Up Your Simulation Game.”
Now we could discuss simulation more, but there are lots of resources discussing the role of simulation in closing the theory-practice gap in nursing. Instead, we’ll take more time to discuss a lesser-known solution.
Using Video Assessment to Bridge the Theory-Practice Gap in Nursing
Another innovative and disruptive software exists that enhances your current simulation program and provides students even more affordable hands-on practice. The tool is video assessment software.
What is video assessment software?
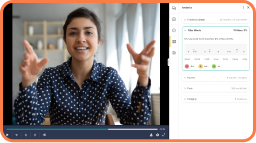
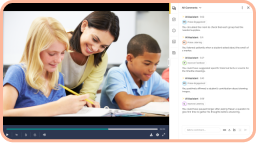
Video assessment software allows students to record or upload videos—anytime and anywhere—of themselves demonstrating a skill. Then the software securely shares these student videos with professors, TAs, or peers so they can document, assess, and give time-stamped feedback for skill competency.
Similar to simulation, video assessment leverages cutting-edge educational technology to spur experiential and evidence-based learning. It literally fits three of the four tactics that the NCSBN recommends. For similar reasons, Dr. Ali Galindo believes video assessment software, like GoReact, helps bridge the theory-practice gap in nursing. Listen to the short clip below to hear what Dr. Galindo’s thoughts.

How Video Assessment Makes a Difference
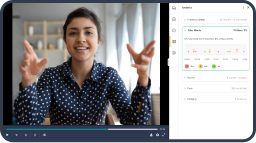
Seeing video assessment in action best illustrates the power and possibilities. In this short clip, Dr. Galindo shares a student’s feedback-rich experience performing a sterile skill check-off.

As you can imagine, nursing programs continue to expand their use cases for video assessments to prepare new nurses. Many programs use the software to enhance debriefing sessions from their high-tech simulation labs. To take advantage of the advanced feedback features, they simply upload simulation videos directly into the software.
To also give students more opportunities outside the high-tech simulation lab, programs ask students to record skills check-offs, patient education exercises, collaborative SBAR assignments, and more.
This augments the heavily booked simulation labs and provides students with more practice and rich feedback on psychomotor and soft skills. In this example, Dr. Galindo asks students to do a mental health history video assessment to help her candidates hone communication skills.

Hopefully, these examples get you thinking about all the different ways you can use simulation and video assessment to better prepare new nurses. There’s a lot you can do with these two to better prepare nursing students for clinical practice. That being said, while simulation and video assessment can help a lot in preparing new nurses for that first day of work, we still need a bigger and better bridge to cross this gap.
Will These Solutions Solve the Problem?
A few years ago at the National Nurse Educator Summit—back when in-person conferences existed and thrived—the session leader spoke like a revolutionary in her presentation, “Hot Topics in Nursing Education.” She saw the theory-practice gap in nursing for what it is: a systemic problem. Citing Lewin’s Change Theory, she gave examples of the kind of disruptive questions we’d need to ask to make systemic structural changes.
This makes sense. While simulation video assignments improve the depth of learning for students, the nursing community can’t forget that in order to fully overcome this issue requires structural changes. And those structural changes also need to be collaborative. 
The Imperative Role of Collaboration
Remember that literature review? The article organized past solutions for the theory-practice gap in nursing by type of institution. As nursing programs brainstormed solutions from their end, the healthcare facilities hiring new nurses independently tried a few things too. But to truly bridge the gap, there needs to be a collaboration between nursing programs and healthcare providers working together.
The necessity of collaboration is best illustrated by this little nugget from a study by The Nursing Executive Center of the Advisory Board Company.
“When nursing educators were asked if their graduates were ready to practice, 89.9% said they were. When the managers were asked if those new hires were ready, only 10.4% of nurse executives felt that these new graduates were prepared.”
This very fractured line of communication sparked a heated discussion at an NNES conference a few years ago. A panel of nurse educators and executives gathered for a special session on “Clinical Judgement: The Bridge Between Education and Practice.” As you can imagine, the two sides—both frustrated—agreed on little.
Some of the panelists prioritized teaching nursing graduates psychomotor skills to the point they could do any skill check-off in their sleep. Some nurse executives worried less about skill proficiency and wished to prioritize clinical judgment.
However you read it, this special conference session underscored the lack of communication and coordination between nursing programs and healthcare providers.
Luckily an epiphany took place before the temperature rose too high. An audience member raised their hand and explained how her state recently brought together educators, government, and nursing executives to define expectations and standards. You could feel the heads nodding around the room. “Yes!” everyone seemed to say—“we need more collaboration and communication.”
The Key: Collaboration, Simulation, and Video Assessment
While research shows that tools shorten the gap, today new leaders in the nursing community call for more. More structural changes. More collaboration. After all, it takes more than tools and new technology to demolish this decades-long plague.
So if you’re tired of hearing about the theory-practice gap in nursing, think big structural changes and collaboration. Get together your local, regional, or state nursing programs and healthcare providers to start talking.
And while nursing programs and providers plan that bigger and better bridge, continue to utilize simulation and video assessment. Let’s be honest, whatever structural plan the nursing community adopts to close the theory-practice gap in nursing, the plan will surely star simulation and video assessment. (How could it not?!)
To learn more about preparing new nurses with video assessment, download Increase New Nurses’ Clinical Judgment or watch Closing the Theory-Practice Gap in Nursing with Video Assessment.