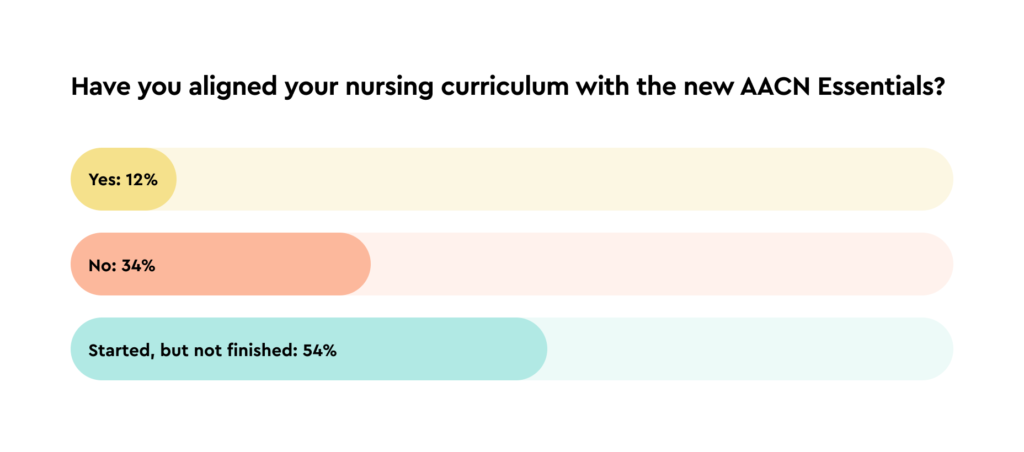
For nurse educators everywhere, 2024 marks the deadline for implementing the new AACN Essentials. For some, this looming deadline may seem like more than enough time, but for others, it may leave you wondering where to even begin. In a recent poll, we found that 34% of nurse faculty had not begun the process of integrating the new Essentials into their nursing program, and another 54% had started but not completed the alignment. Whether you’re well on your way or aren’t even sure what the new Essentials entail, here’s a 3-step process to follow.
Why the AACN Essentials Matter
The update to the Essentials and shift to a competency-based education (CBE) model reflect the needs in today’s healthcare environment. Demand for skilled and workforce-ready nurses is projected to be at an all-time high of 1 million new nurses by 2030. Higher ed programs are a critical pipeline to supply and strengthen the core of skilled nurses.
These accelerating and compounding healthcare needs require new solutions and adapting new approaches to recruiting, educating, and assessing future nurses to ensure that they have the skills and tools required to address the healthcare challenges. To bridge the gap between education and practice, these new Essentials are designed around 10 domains, each carrying competencies and sub-competencies, as well as eight foundational concepts. This new model provides clarity and consistency in nursing program outcomes and establishes the standard for graduates to demonstrate their abilities and transition more effectively into practice.
Shifting to Competency-Based Education
The new Essentials shift the focus to knowledge, skill and competency development, and assessment across all nursing degree programs. Competency-based education is a model where students prove mastery of skills and in turn requires faculty to adopt new strategies to assess and provide feedback to students. Competency-based education allows a student to express what they’ve learned by performing or demonstrating an action that is observable and measurable. It also allows students to advance at their own pace based on their ability to master a skill, making the learning environment more personalized and convenient for students across all degree levels. Nurses enter the profession more prepared to practice and healthcare organizations have clearer, consistent, and confident expectations of these new nurses’ skills.
Having followed a competency-based model since the 1970s, Alverno College nursing faculty know firsthand how this approach benefits their students and faculty.
- Learner centered (not teacher centered)
- Improved quality of learning
- Expanded access for non-traditional students
- Improved workforce readiness
- Competency clarity (students understand goal)
- Connection with student-centered missions
- Competencies change
- All students benefit equally
If you, like Alverno, are already practicing competency-based learning you may be a step ahead, but you still have actions to take to ensure the competencies and sub-competencies of the new Essentials are embedded in your nursing curriculum.
Let’s get started …
1. Collaborate for Change
First, we must focus on our people and make sure we involve faculty in the process. They are, after all, the implementers and evaluators of the curriculum so they should be involved at the beginning and throughout the process as much as possible.
Consider forming an Essentials task force, made up of cross-specialty faculty and including veteran and rookie educators to get a diverse perspective. Task force members can serve as ambassadors throughout your program to promote the changes, serve as trainers, and provide feedback to the core team throughout the implementation.
Equip this team with the resources they need to be successful. This includes time and departmental support to focus on the Essentials integration, and competency-based learning and assessment resources.
Remember that change is hardest on people and takes time. Involving the right people in the process can ease the pain. At the beginning and throughout the process, remind faculty of the purpose of the change—to better prepare nursing students for tomorrow’s healthcare jobs. Encourage the team to view the change as an opportunity to meet the new challenges in healthcare with fresh and innovative approaches to learning.
“The faculty will see that this does take a significant amount of work to create the learning experiences and the assessments, but once you do there is a huge return on investment, and that’s what you need to explore together as a corporate faculty,” —Peg Rauschenberger, Alverno College (WI)

2. Map Your Curriculum to the New Essentials
The second step in the process is probably the largest undertaking, and can be broken into phases.
- Evaluate existing curriculum. Once you have your core team together, take a look at your existing curriculum. Often this can seem like the most daunting step. The current curriculum is familiar to the team, and likely developed by the same people now evaluating it. It’s important to understand and relay to your task force that implementing Essentials doesn’t mean you’re starting from scratch. Programs may have a lot of the components already embedded in their curriculum, which will be discoverable through the process.
- Map courses to the new domains. Through the evaluation you’ll begin to see how your existing courses align with the new domains in many areas. The new curriculum shouldn’t mirror the new domains and concepts; rather these should be layered within the new curriculum. Your team will be able to identify existing learning experiences and activities that already address the competencies, as well as begin to brainstorm new additions. This approach allows programs flexibility and innovation in designing their curriculum within the guidelines of the Essentials.
- Identify gaps. Once you’ve crosswalked your existing curriculum to the new competencies, it will be evident what’s missing. When you identify what isn’t covered in your current curriculum, you can develop learning strategies and assessments within courses to ensure you’re meeting program outcomes.
3. Design New Assessment and Feedback Strategies
As you evaluate your assessment strategies, remember that the focus should be on evaluating students’ ability to translate skills from the classroom into practice. Assessment methods can take various formats, but the end goal is the same—to accomplish more intentional evaluation of knowledge and skills to provide greater consistency and preparation for graduates.
Traditional assessments focus on grades and transcripts and evaluate a student’s progress but don’t measure competency or real-word application. In a competency-based model, the purpose of assessment isn’t just to give a grade, but to allow students the opportunity to demonstrate competency through both formative and summative assessments.
Feedback that is meaningful and actionable is a critical component of effective assessment. Feedback should be frequent and specific on what skills are well-developed and which need further development.
“You will have clear data that will demonstrate how well your students are meeting your overall program outcomes. This data is much more in depth than just exam scores.” —Peg Rauschenberger, Alverno College (WI)
For some educators, transitioning from traditional practices toward this new model can be daunting. It’s important to provide support with resources and tools to help facilitate the transition.
No matter where you are on the path toward meeting the new Essentials, with the right tools and resources, you will get to the finish line. Hear from two nursing faculty on their process and best practices.

If you’re already a few steps into the process, share your ideas, examples, or tips with other nursing faculty.
Don’t miss the next step in AACN Essentials implementation: Tackling Curriculum Transformation.